
USask provides virtual care during pandemic
When an outbreak of COVID-19 caused travel restrictions to be instituted in northern Saskatchewan in May, residents’ access to health care services were limited—especially for expectant mothers.
By Kristen McEwenA University of Saskatchewan (USask) team found a way to utilize existing technology to provide prenatal care for pregnant women who were unable to leave the community of La Loche due to the lockdown.
“Virtual care has come to the forefront because patients can’t see their physicians in person,” said provincial department head of surgery Dr. Ivar Mendez (MD) of USask’s College of Medicine. “One of the issues we were confronted with was how to provide prenatal care to pregnant women who needed ultrasounds when there’s no ultrasound system in La Loche.”
More than 30 women were in need of prenatal ultrasounds during the lockdown in La Loche, located nearly 600 kilometres northwest of Saskatoon.
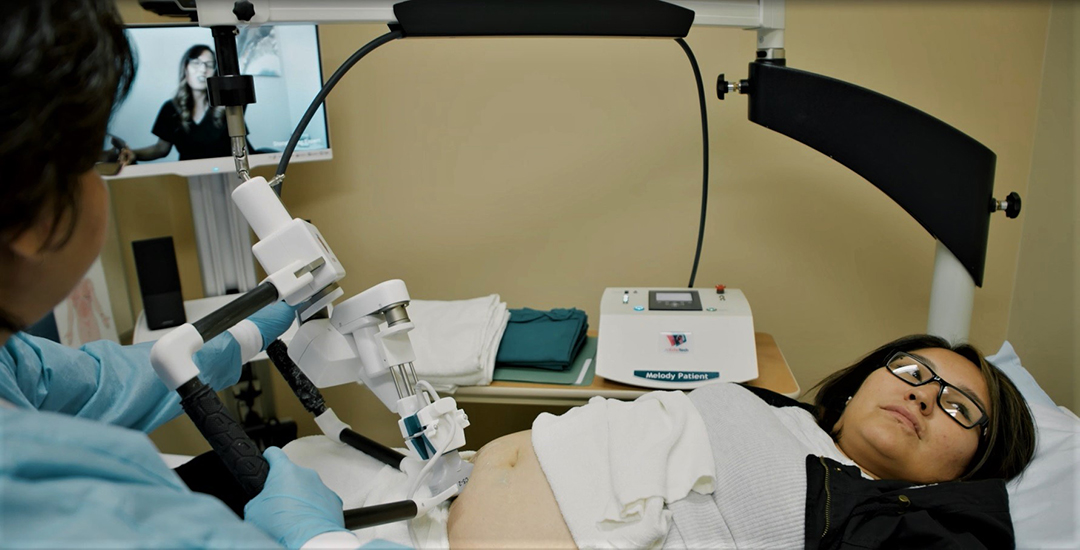
Fortunately, Mendez and his team were able to quickly deploy a prenatal tele-robotic ultrasound system to provide care for acutely ill patients, children and expectant mothers. The technology provided patients with the diagnostic services needed, without increasing their risk of exposure to COVID-19 by travelling to Saskatoon.
Mendez and the research team pioneered the use of this novel technology three years ago in a research project in Stony Rapids, Sask. They have been using this technology in northern remote Saskatchewan communities ever since. The multidisciplinary team is composed of Drs. Scott Adams (MD), Paul Babyn (MD) and Brent Burbridge (MD) from diagnostic imaging, ultrasound technologists Nadine Kanigan and Shawna Piche and Dr. Veronica McKinney (MD), director of Northern Medical Services.
When residents need an ultrasound, they go to their local clinic and a technician connects via video conference with a sonographer in Saskatoon who can manipulate the robotic ultrasound probe remotely.
In La Loche, some of the ultrasounds conducted were critical in determining patients’ treatment, and even saving pregnancies.
“The big risk was the women travelling individually to Saskatoon,” Mendez said. “They could have contracted COVID-19 because both mother and child were particularly vulnerable.”
From finding child care to travelling for hours, it was challenging for pregnant women to leave their community to receive the health services they needed, Mendez added.
“It was clear that it was a great advantage to our patients to not leave their community and have the ultrasound done in their own community,” he said.
In the midst of the pandemic, virtual care has become a necessity for patients in remote communities—especially in the case of prenatal care.
As a result of this experience, there are plans for ultrasound system health services to be available in several remote northern communities in the future, Mendez said.
“We demonstrated we can provide an important diagnostic service in the middle of an area where COVID became an outbreak, and also provided the prenatal care that mothers need,” Mendez said.
Being able to use this technology as a viable way to provide diagnostic care during the pandemic to underserviced and remote populations would not have been possible if the research program hadn’t already been in place at USask, Mendez said.
The basic research that took place was necessary to develop the technology, supported by the Saskatchewan Centre for Patient-Oriented Research, and the Saskatchewan Health Research Foundation.
“Once this pandemic is over, whenever that’s going to be, virtual care is going to be a mainstream way for us to provide health care to the population, not only in Saskatchewan, but the world,” Mendez said.
The Robotic Ultrasound equipment that was deployed in La Loche was financed by Leslie and Irene Dubé via the Royal University Hospital Foundation.
