News
Loading...
Events Calendar
Loading...
About Us
The Department of Psychiatry offers medical undergraduate and postgraduate residency as well as postgraduate training in Master’s, PhD and postdoctoral fellowship opportunities in neuroscience and applied psychiatry. We also offer an ongoing series of continuing professional education activities. Our research reflects the diversity of our faculty and includes clinical, basic biomedical\applied research in psychiatry and neuroscience.
A vibrant group of psychiatrists provide clinical services on an inpatient and outpatient basis. We have medical faculty throughout the city offering general adult, child and adolescent, forensic and geriatric services as well as many other subspecialized clinics. We are committed to pursuing high quality academic and clinical service provisions in the context of providing our patients and the people of Saskatchewan with excellent and compassionate care and a new generation of well-trained clinicians, educators and researchers. Thank you for visiting the website!
Dr. Adekunle Garba (AG) Ahmed, MBBS, MSc, MPsychMed, LLM, MRCPsych, FRCPC
Professor and Provincial Head
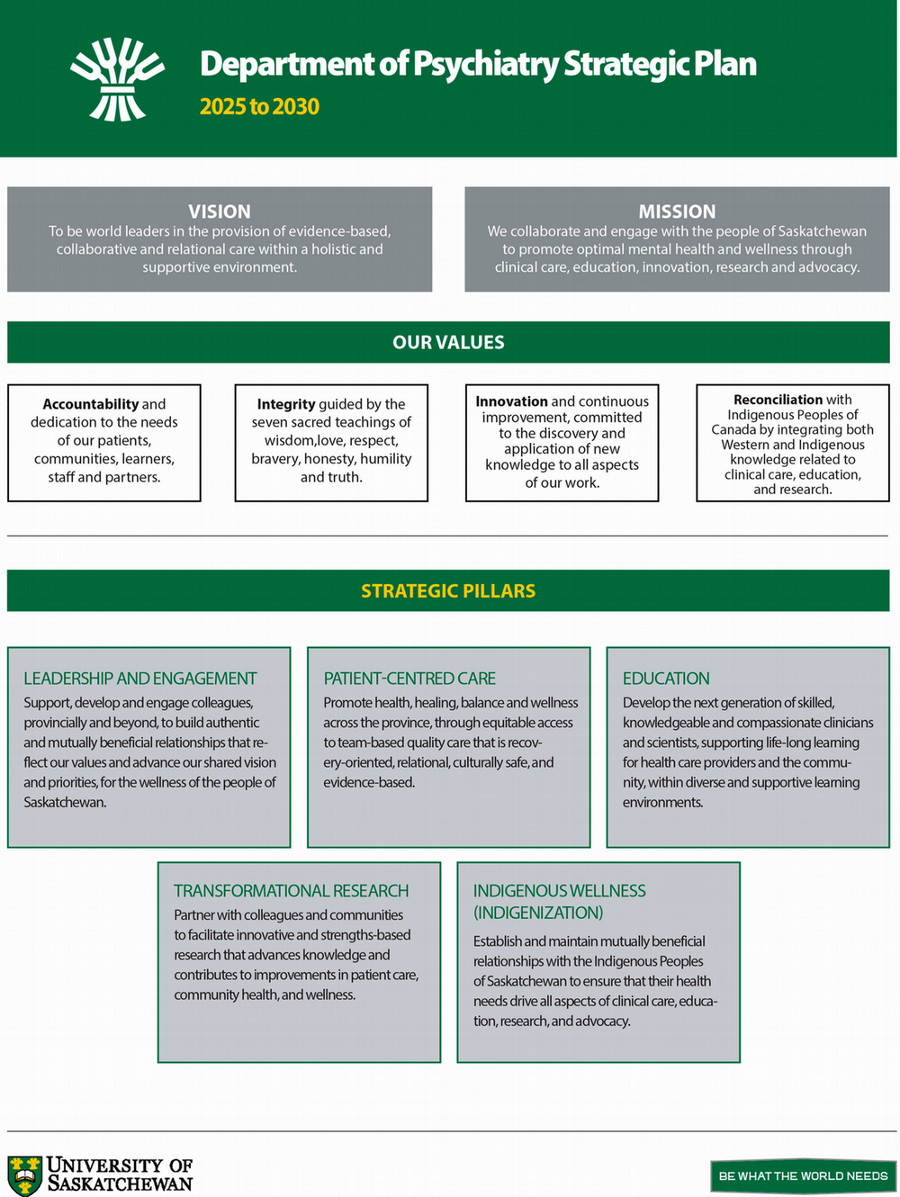
Our Vision
To be world leaders in the provision of evidence-based, collaborative and relational care within a holistic and supportive environment.
Our Mission
We collaborate and engage with the people of Saskatchewan to promote optimal mental health and wellness through clinical care, education, innovation, research, and advocacy.
Values
Accountability
Integrity
Innovation
Reconcilliation
Purpose
The department of psychiatry is a unified organization with a membership that includes medical staff of the Saskatoon Health Authority as well as faculty based out of the University of Saskatchewan and surrounding community. Guided by leadership of a provincial head, members work collaboratively with dedication to excellence in clinical service, education, and research. With a mandate to support province-wide programming, the department nurtures partnerships in the field of mental health and addiction services, and strives to enhance academic activities and patient care through affiliated clinical programs.
Education
Welcome to our education programs in Psychiatry. We provide a full spectrum of education experience in Psychiatry beginning with an undergraduate medical curriculum, followed by the opportunity to complete specialty training in a fully accredited Royal college program in Psychiatry. Our Psychiatry postgraduate residency is a five year program offered at Saskatoon and Regina sites. We also have a sub-specialty program in Child & Adolescent and Forensic Psychiatry.
We provide Psychiatric training for Residents from other programs in Family Medicine, Pediatrics, Emergency Medicine, and elective opportunities for other specialty programs. The Family Medicine Resident clinical experience is highly regarded by the trainees and Department of Family Medicine.
Additionally, the Department also provides a broad spectrum of Continuing Professional Development curriculum from September to June. Please follow the section links under Education to learn more about our programs, and for additional contact information.
Dr. Malin Clark, BA, MD, FRCPC
Education Director
The General Objectives for the Undergraduate Medical Program are outlined in the following document.
The mistreatment, discrimination, and harassment policy is a key document to read and refer to for faculty and students to ensure a safe working and learning environment.
Psychiatry is a core program within the undergraduate medical curriculum. Pre-clerkship (years 1 and 2) includes multidisciplinary lectures and small group sessions which include members of the Department of Psychiatry as part of the learning experience.
There are also opportunities for students in this part of their training to “shadow” clinicians in their offices or in the hospital. For information on how to organize “shadowing” contact the Psychiatry Undergraduate Office as listed below.
Mental Health Foundations and Clinical Skills in the last half of year 2 provide the first formal opportunity for undergraduate medical students to learn about psychiatric illnesses and perform a psychiatric interview with real patients. These courses are a combination of didactic and small group teaching, which take place concurrently.
Clerkship
The clerkship syllabus is described here, with Psychiatry beginning on page 74.
Psychiatry is one of the core clerkship rotations. Psychiatry provides a 6 week core rotation for all Year 3 medical students. In addition we also provide electives for all students interested in furthering their experience in Psychiatry. The clinical clerkship is situation at three sites, which include Saskatoon, Regina and Prince Albert.
The goal is to provide a varied and exciting experience in Psychiatry. We are fortunate enough to have one of the most varied programs in the country with opportunities that include: adult psychiatry, child psychiatry, consultation liaison psychiatry, geriatric psychiatry, forensic psychiatry, inpatient/outpatient care and emergency psychiatric services. In addition to the clinical exposure and training, there are seminars and tutorials from many of our dedicated consultants and psychiatry residents. This experience often includes one-to-one clinical teaching by faculty and residents. Evaluations occur through One-45 and include a mid-term and final evaluation.
For more information on our clerkship or setting up an elective, please contact our Undergraduate Medical Office:
Danielle Gage
Undergraduate Medical Education
Postgraduate Subspecialty Programs
Tel: (306) 844-1312
Fax: (306) 844-1504
The Residency training program at the University of Saskatchewan is a Royal College of Physician and Surgeons accredited five-year program designed to prepare trainees to practice general adult psychiatry, or prepare trainees for subspecialty training. Our strengths include dedicated and engaged teaching faculty, cohesive resident cohort that actively participate in program development and review, and a diversified, distributed learning experience.
The residency training program is distributed across our Saskatoon and Regina campuses, and there are also opportunities for rural and remote learning. Our smaller program size fosters an environment of collegiality and provides residents with an approachable faculty encouraging of residents’ independent learning needs. This also gives residents opportunity to actively participate in program renewal and growth through participation in curriculum review and operational committees.
The Department currently has two Royal College accredited subspecialty programs, Forensic, and Child & Adolescent.
To learn about our residency program in detail, please explore the Residency Training Program (PGME) section.
|
Dr. Dawn De Souza |
Dr. Madhav Sarda |
|
|
Dr. Nishma Patel |
Dr. Fiyin Peluola |
|
|
Program Administrators | pgme.psychiatry@usask.ca |
|
|
Saskatoon: Nadine Loran 306-844-1080 |
Regina: Mercedes Williams 306-766-3177 |
Welcome to our Master’s and Ph.D. graduate programs administered through the Health Sciences program centrally in the College of Medicine. We have expertise in clinical psychiatry, Applied Research, Biological Psychiatry and Aboriginal mental health.
The graduate program in Applied Research focuses on the psychosocial determinants for emotional and physical wellbeing, and for mental health issues as well as the distribution and the effectiveness of treatment of these mental health issues.
The graduate program in Biological Psychiatry focuses more on determining the biological basis for brain dysfunction in selected mental health issues, particularly depression. Most of these studies are based on animal and cell models, and are designed to investigate the effect of pharmaceutical treatment(s) on cell function and/or the animal’s behaviour.
Research in Aboriginal Mental Health occur under the direction of a medical anthropologist.
While many of the studies in both the Applied Research and the Biological Psychiatry programs are undertaken by graduate students and technicians, more independent studies are taken on by post-doctoral researchers training for a career path in Academia or Industry. Interest in a concurrent M.D/M.Sc. (or Ph.D.) program can also be accommodated within the College of Medicine’s M.D. curriculum.
For more information on the Health Sciences Graduate Studies program or email our office.
We have a vibrant array of continuing educational activities in the Department of Psychiatry. Each month we have two departmental grand rounds and one journal club. We strive for balance and scope in the choice of topics and presenters. In addition to the traditional format, some grand rounds are part of the Debate series, modelled after the Maudsley Debates and recently championed by colleagues at Dalhousie. Two resident-consultant pairs debate each other on mental health topics and the pair that sways the most audience votes wins. Another popular format is the Second Opinion series: a panel of experts address questions submitted by the audience, both ahead of time and on the spot. Collaboration is encouraged among disciplines and within the department. The rounds are available through Telehealth and WebEx to our other teaching site in Regina and remote sites in the Saskatchewan Health Authority. Members are encouraged to develop Personal Learning Projects around the topics of grand rounds, assisted by pre-rounds literature resources suggested by the presenters, for Royal College, Maintenance of Certification, Section 2 credits. This past year, we developed a workshop on the Clinical Assessment of Capacity, led by Drs. Baillod and Thorpe, that was accredited for Section 3 credits.
Planning for the annual Academic Day is underway. The planning committee, made up of psychiatry clinicians and researchers, psychologists, and representatives from Mental Health Services, considers the input from target audience members and other perceived learning needs and determines the theme, content, and choice of speakers for the event.
Dr. David Porter
Director of Continuing Medical Education
Residency Training Program (PGME)
Please explore the tabs below to learn about our residency training program.
Psychiatry as a specialty transitioned to the Royal College of Physicians and Surgeons of Canada Competency by Design (CBD) Framework on July 1, 2020. Residents who enter the program will follow the CBD curriculum.
Psychiatry residency in CBD is composed of 4 stages of training.
This brief stage focuses on orientation to the program and assessment of new trainees to ensure they have the basic skills necessary to move on to the Foundations of Discipline stage. In psychiatry, these basic skills include taking a psychiatric history and accurately communicating clinical encounters.
The first two blocks of PGY1 include 1 block of ER Psychiatry and 1 block of inpatient psychiatry. The Residents participate in a Resident Boot Camp which includes orientation to the program, site and specialty of psychiatry.
This stage covers broad-based competencies that are necessary before moving on to more advanced competencies. This stage corresponds with Junior Resident status in the traditional model. Foundations encompasses the remaining blocks of PGY1 and PGY2. In psychiatry, the training experiences (or rotations) in Foundations include the medical rotations and the general adult inpatient and outpatient rotations. The competencies that the residents are expected to achieve are generally of lower complexity than the competencies in the Core and TTP stages.
The remaining 11 blocks of PGY1 are comprised of:
- 2 blocks of Psychiatry ER
- 1 block of Consultation Liaison Psychiatry
- 1 block of Internal Medicine (CTU)
- 1 block of Neurology
- 1 block of Emergency Medicine
- 1 block of Family Medicine
- 1 block of Geriatric Medicine
- 1 block of Psychiatry Selective (Adult Psychiatry, Consultation Liaison Psychiatry, Child and Adolescent Psychiatry, Geriatric Psychiatry, Forensic Psychiatry, and Rural/Underserved Psychiatry)
- 1 block of Medicine Selective (Internal Medicine (CTU), GIM, Other Internal Medicine Subspecialty, Family Medicine, Emergency Medicine, Geriatric Medicine, and Neurology)
- 1 block of Elective/Research
Core of Discipline
This stage covers the core competencies that make up the majority of the discipline. This stage corresponds with training experiences include Child Psychiatry, Geriatric Psychiatry, Severe and Persistent Mental Illness (SPMI), Addictions, Psychotherapy, and other rotations. The competencies achieved in this stage may be similar to those in Foundations, but are at a higher level of complexity. This stage encompasses PGY3 and 4 years. The proposed training experiences for PGY3 and 4 are:
PGY3
- 6 months of Child and Adolescent Psychiatry
- 6 months of Geriatric Psychiatry
- 2 months of Consultation Liaison Psychiatry
- 1 month of Addictions Psychiatry
- 2 months of Acute Care Psychiatry
- 1 month of Consolidation
- 6 months of Severe and Persistent Mental Illness
Transition to Practice
In this stage, the resident should demonstrate readiness to make the transition to independent practice. The Resident consolidates the CanMEDS competencies with an emphasis on career track determination. Residents assume greater leadership roles in teaching, program administration and work in advanced clinical rotation environments. This stage corresponds to the PGY5 year. The proposed rotations for PGY5 include:
PGY5
- 3 months of Inpatient Psychiatry or ER Psychiatry or another Psychiatry Training Experience where the resident leads the team.
- 3 months of Selective training in an area that pertains to psychiatry
- 6 months of elective
The University of Saskatchewan psychiatry residency program has a provision for a six-month elective that can be taken in any area relevant to contemporary psychiatry and/or research. The entire elective may be completed outside of Saskatchewan with the approval of the Residency Training Committee and Postgraduate Office of the College of Medicine. Six months of electives provide the opportunity for additional training specific to psychiatry.
Community Based Training Experiences
Many of the clinical rotational experiences have community oriented training opportunities available. Residents are supported to further explore rural experiences through rural clinics. PGY2 residents are required to complete four rural clinics during their residency training.
The Saskatoon Department of Psychiatry has a Northern Medical Services Psychiatry Clinic, which provides remote and fly-in psychiatry services to three communities in Northern Saskatchewan – La Loche, La Ronge and Stony Rapids, for both children and adults.
During the five years (PGY1-5) there is a comprehensive formal teaching program consisting of:
- Core Seminar curriculum beginning in PGY1.
- Psychotherapy seminars plus longitudinal individual psychotherapy training and supervision in CBT, Dynamic, DBT, and IPT.
- One year of Family therapy training inclusive of seminars and direct Family therapy training and supervision.
- Interviewing skills course including Mock STACERs.
- OSCE course PGY2-5.
- Critical appraisal and research curriculum as part of Academic Half-Day seminars.
- TIPS (Teaching Improvement Project Systems). This is a course that PGY1 residents must attend.
During a Resident’s five years of training, they will develop skills in diagnostic interviewing, comprehensive assessment, biopsychosocial formulation, use of psychotropic medications, and use of ECT.
Performance Assessments
Residents receive formal performance assessments based on CanMEDS roles and competencies following each block in PGY1 and at quarterly intervals during PGY2-5 based on the rotation plans competencies. Residents are assessed utilizing stage specific Entrustable Professional Activities (EPAs). The Competence Committee reviews each Resident at minimum every six months based on multi-source performance assessments that include, but are not limited to training experience ITARs, emergency on-call assessments, multisource feedback from allied health professionals, written and OSCE examinations. Performance evaluation is based on the CanMEDS competency framework.
Examinations
- Annual OSCE exam held each spring for residents in PGY2-5.
- COPE exam: National written MCQ exam each year to provide residents (PGY1-5) with formative feedback of knowledge based on national benchmarks.
- PRITE exam: Written exam bi-yearly to provide residents (PGY2-5) with formative feedback of knowledge based on national benchmarks (U.S. based exam)
Continuing Education
Departmental Grand Rounds, Quality Improvement Rounds, Department of Psychiatry Academic Day, Journal Club, Visiting Professor Rounds and Workshops are organized as part of Continuing Education.
Journal Club is resident led and residents have the opportunity to facilitate journal club presentations during residency training.
The Visiting Professor Program is particularly active, bringing in distinguished visiting faculty each academic year. In addition to presenting at Grand Rounds, the visiting professors meet with the residents informally and present workshops, primarily attended by the residents.
Quality Improvement Rounds or Mortality and Morbidity Rounds are held monthly in Saskatoon and Regina, which include discussion of patient deaths and of patients who suffer significant treatment complications or who are refractory to treatment. Residents will be involved in the presentation of the patient if they were involved in the care of the patient during the event discussed.
Residents are expected to present at Grand Rounds and Quality Improvement Rounds during their residency.
The Department of Psychiatry Academic Day is held yearly, usually in Saskatoon. Residents at both sites are provided with protected academic time to attend.
Clinical training in various psychotherapies plays an integral role in the program. All residents are expected to achieve a range of competencies in many forms of psychotherapy as required by the Royal College of Physicians and Surgeons of Canada.
In PGY2, residents are supervised in supportive psychotherapy. They are provided with a psychotherapy supervisor who provides supervision of at least two cognitive behavioral cases for a minimum of 20 hours. PGY2 residents also participate in a foundational curriculum focusing on an introduction to CBT and Psychodynamic Psychotherapy.
PGY3 residents participate in family therapy. Residents must observe or co-facilitate a minimum of one psychoeducation or therapeutic group.
In PGY3-4 residents participate in a two-year rotating curriculum focusing on advanced topics in psychotherapy such as CBT, Psychodynamic Psychotherapy, formulation, motivational interviewing, and personality organization.
PGY3-5 residents are supervised in psychodynamic psychotherapy. They must complete a minimum of 60 hours of psychodynamic therapy as a primary therapist. Residents must complete an additional 20 hours of supervised training in a psychotherapy modality of their choice: CBT, Psychodynamic Psychotherapy, IPT or DBT, or another evidence-based psychotherapy where they act as the primary therapist.
In keeping with the RCPSC recommendations, residents participate in research and scholarly projects during the course of the residency. A research curriculum is offered as part of the PGY1 academic day curriculum. Residents are provided with protected time in PGY2 to complete a junior research project which consists of a narrative literature review. Residents complete a senior research project which includes participation in a scholarly research, quality assurance, or educational project relevant to psychiatry. Residents are expected to present a poster of their research at the Saskatchewan Psychiatric Association Annual conference, and also have opportunities to present their work at local, national and international conferences. A faculty research coordinator and a research facilitator supports resident research at both sites.
Emphasis is placed on collaborative research models and is facilitated by a Faculty Resident Research Coordinator. Opportunities for research collaboration exist with clinical faculty and also with basic science faculty.
Saskatoon residents acquire clinical experience in emergency psychiatry (Jim Pattison Children’s Hospital ER), inpatient services at the Irene and Leslie Dubé Centre for Mental Health and outpatient services at Royal University Hospital, the Mental Health Clinic, The Regional Psychiatric Centre and in private downtown offices. Residents acquire experience in consultation services to other departments at Royal University Hospital, Saskatoon City Hospital, and St. Paul’s Hospital, as well as to local schools and courts. Residents also gain experience in community settings through Mental Health Rehabilitation Services, Community Psychiatric Nursing and the McKerracher Centre (Day Program). Much of the experience in Geriatric Psychiatry is in various long-term care facilities and nursing homes throughout Saskatoon.
Residents gain experience in working with a number of community agencies in Mental Health such as the Crisis Intervention Service, Addictions Services, Canadian Mental Health Association, the Youth Resource Centre, Early Intervention program, the Clozapine Clinic and Anxiety and Mood Disorders Program.
Residents based in Saskatoon or Regina may have the opportunity to undertake core rotations and/or senior selectives at the other site during their training experience between PGY1-5.
Regina provides training under a distributive learning experience with the College of Medicine office, and Site Director, Dr. N. Patel. Regina has had CARMS specific positions since July 2010. The University of Saskatchewan Psychiatry program at the Regina site provides the full spectrum of training requirements for residents.
Residents based in Saskatoon or Regina may have the opportunity to undertake core rotations and/or senior selectives at the other site during their training experience between PGY1-5.
What are the advantages of Training at the University of Saskatchewan?
- Collegial, friendly and supportive environment including a cohesive and engaged resident cohort with four residents per cohort year in Saskatoon and three residents per year in Regina
- Dedicated faculty who are approachable, enthusiastic and effective teachers
- Residents that prefer a smaller, ‘family-oriented’ program will thrive in the close-knit program
- Small program that allows for 1:1 teaching experiences and mentorship
- Program is supportive of individual learning goals and responsive to resident professional and personal needs
- Dedicated resident space including a newly renovated teaching space equipped for virtual learning, lounges, and individual resident offices in Saskatoon
- Residents are given a half- day per week of protected academic time plus an additional week dedicated to research and study every six months
- Residents hold retreats in June and December each year focused on team building and wellness
- Psychiatry residents are provided with funding and support to attend conferences, courses and present research during the course of their residency:
- $1000 per year per resident to use toward education materials, electives, conferences and travel
- Supplemental Travel: $2000 to each resident during the residency term to support residents who are presenting at conferences (not just attending)
- Ottawa and London review course registrations for Royal College licensing exam preparation
How are residents involved in the program?
The residents have a strong voice in shaping the program. They play an active role in program curriculum development with representation on the resident training, Competency by Design, and research committees. To ensure ongoing resident safety and contract support, residents also contribute to the department safety committee and Resident Doctors of Saskatchewan. Constructive feedback and communication are strong suits of the program through monthly resident-only forums followed by a resident administration meeting with the Program Director.
What are the work hours and call frequency?
Residents generally work from 8:30-9:00 am to 5:00 pm, with the exception of two days per week when the residents meet for morning teaching rounds at 8:00 am or when they are administering ECT during their PGY2 adult inpatient rotation. PGY1 and PGY2 residents do four call shifts per month with PGY1 residents buddied with an upper year resident for at minimum the first three months of PGY1. PGY3-5 residents do three call shifts per month.

What is the salary of a resident in Saskatchewan?
Residents’ salaries are determined by the Resident Doctors of Saskatchewan Collective agreement. Resident doctors are remunerated through salaries, call stipends, and stat holiday pay. Current salaries are listed below.
- PGY1 $59,234
- PGY2 $64,599
- PGY3 $69,959
- PGY4 $75,296
- PGY5 $80,594
- PGY6 $85,879
Our program residents talk about our program and answer some common questions.
Why did you choose psychiatry?
Why did you choose USask?
How are you supported by the program?
What do you appreciate about the learning opportunities in the program?
Eligible CMG and IMG candidates are encouraged to submit CaRMS applications for consideration of a psychiatry residency position. For details on how to apply to our program, please visit the CaRMS website.
Candidates short-listed for an interview will be notified by email with a letter of offer to interview.
Child & Adolescent Subspecialty
The University of Saskatchewan offers a two-year program in Child and Adolescent Psychiatry that is fully accredited by the Royal College of Physicians and Surgeons of Canada. The site of training can be either Saskatoon or Regina, depending on the resident’s preference along with the capacity at each site. Note that residents in Regina will have to go to Saskatoon for one mandatory rotation, for which accommodations can be provided.
Child and Adolescent Psychiatrists in Saskatchewan are a collegial group of dedicated psychiatrists who offer a broad range of clinical services. There are opportunities for research and our residents have been successful in winning research awards at international conferences. Faculty are very keen to teach and residents are encouraged and supported to develop their unique career interests within the child and adolescent psychiatry subspecialty. There are dedicated child and adolescent psychiatry inpatient units in both Saskatoon and Regina and we have integrated consultation liaison services with the new Jim Pattison Children’s Hospital.
We look forward to welcoming new residents!
Dr. Madhav Sarda
Child & Adolescent Subspecialty Director
This is an exciting time to be training and practicing in Child Psychiatry in Saskatoon! We are receiving enhanced levels of support for collaborative and team-based care, to expand our triage, psychological assessments, and supports for those children who need emergency care for acute crisis.
The Saskatoon Department of Psychiatry works in close partnership with Child & Youth Mental Health & Addiction Services (MHAS), both in patient care and research. Child & Youth has various programs city wide, and also oversees the Dube Centre, an inpatient unit located adjacent to the Department on campus, with 10 dedicated beds for children in a mental health crisis.
The new Jim Pattison Children's Hospital provides state of the art medical care for the departments of Paediatrics, Labour and Delivery, and Emergency Medicine. Child Psychiatry is involved in the care of the children in the hospital who have mental health needs along with other physical health concerns.
Other unique opportunities exist to provide psychiatric care to rural and remote communities, including telemedicine, rural clinics, and fly-in clinics to northern communities.
Saskatoon is a vibrant, active and culturally rich city of approximately 257,000 people, and growing. In Saskatoon residents will enjoy working alongside the scenic South Saskatchewan River, which provides breathtaking views as it flows through the city. For more information on the city of Saskatoon, please visit www.tourismsaskatoon.com.

At the Regina General Hospital is The Adolescent Psychiatric Unit, a 10-bed tertiary care inpatient unit providing patient care through a specialized interdisciplinary team, in addition to a 10-bed Secure Youth Detox. Psychiatric and psychological consultation, counselling and group therapy are provided by the Young Offender Team to the provincial youth forensics facility, Paul Dojack Youth Center. Autism assessments, treatment and case management is provided through the Autism Center.
We have a strong working relationship with our community partners, which includes the Ministry of Social Services, school boards, Ranch Ehrlo Residential Society (which provide services to complex youth with multi-domain psychopathology from all over Canada), and other community based organizations. Regina is small enough to foster such strong inter-agency working relationships, yet large enough to provide a broad variety of strong evidence-based interventions to the residents of our service area.
Regina, the capital of Saskatchewan, is a modern mid-sized welcoming city of approximately 236,000 people “nestled in the heart in the heart of the Canadian prairies.” For more information on the city of Regina, please visit www.tourismregina.com
Please find below our application form in fillable PDF format. All applications for the 2025 academic year are to be emailed directly to Nadine Loran, program administrative assistant, and should be received by September 3rd, 2024. Applications may continue to be accepted on a case-by-base basis.
Forensic Fellowship
The University of Saskatchewan offers a one-year Fellowship in Forensic Psychiatry that is fully accredited by the Royal College of Physicians and Surgeons of Canada. The principal site of training is located in Saskatoon at the Regional Psychiatric Centre. Training is also undertaken at Saskatchewan Hospital North Battleford. The Fellow will also have involvement with the Saskatchewan Review Board and forensic outpatient assessments.
The Forensic Division is an important part of Saskatchewan’s mental healthcare system, which provides both inpatient and outpatient services. The division promotes clinical care, education, research, and advocacy for forensic mental health patients. The Division consists of members from Correctional Services Canada, the Department of Adult Psychiatry, the Department of Child and Adolescent Psychiatry, the Faculty of Law, Saskatchewan Hospital North Battleford, and private practice.
Saskatoon is a vibrant, active and culturally rich city of over 325,000 people. In Saskatoon residents will enjoy working alongside the scenic South Saskatchewan River, which provides breathtaking views as it flows through the city. For more information on the city of Saskatoon, please visit www.tourismsaskatoon.com.
We look forward to welcoming new Fellows!
Dr. Stephen Adams
Forensic Psychiatry Program Director
Research
The Department of Psychiatry has a vibrant research portfolio continually growing through the efforts of our knowledgeable and dedicated clinical, applied and basic research faculty, students, residents and staff. Our mandate is to undertake fundamental and clinical studies to contribute to continuously evolving field of psychiatry and provide the exceptional training environment to the next generation of scientists and clinicians.
We conduct cross-disciplinary clinical, applied and basic research through biological and sociocultural lenses to improve prevention, develop and implement better therapeutic interventions, and enhance care in individuals living with mental illnesses. We collaborate with Indigenous Peoples’ Communities and with Patient Partners to conduct research for improvements in wellness and mental health. Researchers in the Department tackle mental illness across life span utilizing cutting-edge technologies, from psychiatric genetics to computational psychiatry and artificial intelligence.
The Department is home to the following prominent researchers and innovative research programs:
Anger Disorders and Substance Use Research Group - Led by Dr. AG Ahmed, this research is dedicated to pioneering innovative treatment pathways for dysfunctional anger and substance use disorders (SUD). With a focus on understanding the biological mechanisms underlying anger and the effects of successful rehabilitation on the criminal justice system, the work aims to improve outcomes for individuals grappling with these complex issues.
Attachment Research Laboratory – Led by Dr. G. Camelia Adams, The Attachment Research Lab is focused on developing a better understanding of adult attachment characteristics and their impact on mental health, treatment and recovery.
Cell Signalling Laboratory – Director Dr. Darrell D. Mousseau is the Saskatchewan Chair in Alzheimer disease and Related Dementia. His major research objective is to determine what biochemical events are common to depression and Alzheimer disease (AD). He is also examining depression-related targets in models of diabetes (insulin resistance) and in breast cancer.
Computational Psychiatry Group – Led by Dr. Lloyd Balbuena, the group uses data from electronic medical records, national surveys, administrative records, smartphones, and patent and health worker perspectives to investigate a wide range of topics including suicide, mood instability, neuroticism, emotional dysregulation, health services utilization, and social determinants of mental health.
Child Psychiatry Clinical Studies is overseen by Dr. Declan Quinn, Dr. Melissa Denis, and other collaborators, both within and outside of the Department. Research is focused on multiple factors affecting youth and adolescents, such as depression, anxiety, substance use, ADHD, and more.
Educational Research is undertaken by Dr. Marla Davidson. Interest is in the pedagogy for tomorrow’s physicians. Dr. Davidson is an expert in developing innovative teaching strategies and in psychiatry resident training scholar curriculum implementation and evaluation.
Indigenous Health and Wellness research is undertaken by Dr. Holly Graham. She currently holds an Indigenous Research Chair in Nursing awarded by the Canadian Institutes of Health Research (CIHR), Saskatchewan Health Research Foundation (SHRF), and the Canadian Nurses Foundation (CNF). Dr. Graham's research is strength-based with a focus on Indigenous health, mental health, and wellness.
Mitochondrial Genetics and Brain Function: From Cells to Systems – Dr. Mendes-Silva's research focuses on deepening our understanding of the biological mechanisms underlying mitochondrial dysfunction in mental illnesses, such as mood disorders, and translating this knowledge into the development of mitochondria-based prognostic tools and therapies.
Psycholegal and Fetal Alcohol Spectrum Disorder (FASD) Research Laboratory – Dr. Mansfield Mela is a Diagnostic Research Lead for Canada’s comprehensive national Fetal Alcohol Spectrum Disorder (CanFASD). His research program focuses on FASD and the overlap with mental disorder, often including a forensic lens.
Social and Psychiatric Epidemiology Research Group (SPERG) – SPERG’s focus is on social and psychological and epigenetic risk factors for mental illnesses and mental health including the prevention of mental disorders. The group is led by Dr. Carl D’Arcy, who is also the Academic Director for the Saskatchewan Research Data Centre (SKY-RDC).
Dr. G C Adams
- Attachment Style and Awakening Cortisol in Clients with Major Depressive Disorder With or Without Comorbid Social Anxiety Disorder
- The relationship between attachment, treatment compliance, and treatment outcomes in patients with obstructive sleep apnea
- The Relationship Between Attachment, Recidivism and Treatment in Forensic Patients with Mental Illness
- The Impact of Adult Attachment on Treatment Utilization and Costs in Psychiatric Outpatients
- Effectiveness Early Psychosis Intervention Program and the Examination of Risk Factors Interfering with its Use
- Suicide Psychological Autopsy Network Saskatoon (SPANS): Phase One
- Self-Reported Impairment and Quality of Life Information from Children and Adolescents with Psychiatric Symptoms: The Utility of the WHODAS-Child in the Saskatoon Health Region
- Measuring Self-Reported Emotional Regulation in an Inpatient and Outpatient Psychiatric Population
- Child & Youth Psychiatry - Consent to Participate in a Research Database
- Perspectives from Mental Health Professionals about the Potential Expansion of Medical Assistance in Dying (MAiD) to Patients with Mental Illness as a Primary Reason for MAiD
- Health Care Professionals’ Perspectives on Medical Assistance in Dying
Review the documents below to see the research that has been undertaken by our residents and graduate students.
Saskatchewan Psychiatric Association, Resident and Graduate Student Research 2025
Saskatchewan Psychiatric Association, Resident and Graduate Student Research 2024
Saskatchewan Psychiatric Association, Resident and Graduate Student Research 2023
Saskatchewan Psychiatric Association, Resident and Graduate Student Research 2022
Saskatchewan Psychiatric Association, Resident and Graduate Student Research 2021
Psychiatric disorders affect every community worldwide. Access to mental health and addiction services and expanding access to community-based mental health services is one of the priorities of federal and provincial governments in Canada. Psychiatrists and other mental health professionals work together to deliver care that is evidence-informed and responsive to the unique needs of each patient. Advancement in education and research is vital to the success of contemporary health care and necessary for the ongoing development of psychiatry. The stream is a suite of courses (PSIA 870.6 and PSIA 875.3) within the Health Sciences Program developed by the Department of Psychiatry to create knowledge and optimize development of scholarly skills in psychiatry to tackle multiple aspects of clinical research in mental health. The courses offered under Mental Health Stream are unique and attractive for students and medical residents from the Prairie Provinces and across Canada, offering high caliber training in clinical research targeting mental health.
Learn more:
Health Sciences Graduate Program - College of Medicine | University of Saskatchewan (usask.ca)
Research Volunteering Opportunity in the Department of Psychiatry
There are several ways how individuals can volunteer in research in the Department of Psychiatry.
Faculty: College of Medicine faculty who are seeking MD Research Volunteers for research projects are encouraged to submit a project proposal to deans.projects@usask.ca and it will be available for Medical Students on Google Drive. Deadline to apply for Dean's Summer Research Projects is usually in November MD Year-Round Volunteer Research Opportunity.
You can also submit research proposal to the Department of Psychiatry research division research.psychiatry@usask.ca to assist you and guide both involved parties (i.e. a faculty and a volunteer) on administrative aspects of this research initiative. Sometimes department receives inquiries on volunteering activities from MD and non-MD students and the department can facilitate a matching process.
Volunteers: Undergraduate and graduate students or other individuals looking for academic experience in the Department of Psychiatry are welcomed by the Department upon connecting research.psychiatry@usask.ca and providing an up-to-date CV and a short summary of their research interest. A brief interview will be scheduled with a potential volunteer as needed.
The Department of Psychiatry will follow the CoM Volunteer Research Experience Terms and References. A faculty member and a volunteer should also submit a signed copy of Memorandum of Understanding to research.psychiatry@usask.ca and when appropriate (Medical Student) to deans.projects@usask.ca.
Project Proposal, Supervisor Information (Terms & References), Memo of Understanding Forms can be found here under Undergraduate / MD Volunteer.
The Department is looking for talented researchers to join our team.
Collaborative research
If you are a researcher or clinician interested in collaborating with one of our faculty in the Department, please contact them directly. Their contact information is available through our faculty list.
Postdoctoral Fellows
To view opportunities available for post-doctoral fellowships, please visit our university job posting site.
To apply for an opportunity, please follow the application process outlined in the posting. Additional information can be found through the College of Graduate and Postdoctoral Studies.
Graduate students
MSc and PhD degrees with focus in Psychiatry are available through the Health Sciences graduate program offered by the College of Medicine.
Prospective students are encouraged to view potential opportunities on the university job posting site and apply to the Health Sciences graduate program as per program admission guidelines.
Additional information can be found on the College of Graduate and Postdoctoral Studies (link above).
Funding for Graduate students.
Undergraduate students (medical and other disciplines)
Active researchers in the Department accept a limited number of medical undergraduate students through the Dean’s Summer Research Projects program.
Students enrolled in Anatomy and Cell Biology, Biochemistry, Microbiology and Immunology, Physiology, and Pharmacology undergraduate programs are eligible to partake in research training through the Biomedical Summer Research Projects.
Research assistants
Positions as research assistants or coordinators are available periodically and posted on the university job posting site (link above). Please check frequently for the most recent opportunities and application guidelines.
Post-graduate and Residents
Funding
College of Medicine stipends (review the “Health Sciences” section). College of Medicine Graduate Student Award (CoMRAD) and other funding resources.
College of Medicine funding initiatives.
Research Acceleration and Strategic Initiatives (USask)
https://vpresearch.usask.ca/rasi/
For other research related opportunities within the Department of Psychiatry, please contact research.psychiatry@usask.ca.
Clinical
Clinical consultation and continuing medical care is delivered through individual private clinics, the Royal University Hospital emergency department and inpatient units, other health authority facilities, rural clinics, and in specialized programs developed and delivered collaboratively with Mental Health and Addiction Services.
These specialized services reflect the breadth of our physicians’ interests and expertise, as well as the needs of our expanding population. Through this partnership with MHAS psychiatrists participate not only in Mental Health and Addiction Services program development, review and patient/family centred service delivery but also in activities committed to continuous quality improvement.
Requests for psychiatric services are typically initiated by family physicians and other medical specialists and in some instances by other mental health professionals within the specialized programs.
The Department of Psychiatry offers clinical services that span the continuum of care from community to acute care and back, in close partnership with Mental Health & Addiction Services. We have taken, and continue to take, significant quality improvement initiative to improve patient quality and flow.
Clincial Services:
- Outpatient Psychiatry
- Inpatient Psychiatry (Irene and Leslie Dubé Centre for Mental Health at RUH)
- Rapid Access Clinic
- Specialized Services
- Addiction Services (MHAS outpatients & Calder Centre)
- Anxiety and Mood Disorders Program
- Clozapine Clinic
- Consultation-Liaison Psychiatry (RUH, SCH, SPH)
- Early Psychosis Intervention Program
- Maternal Mental Health Program
- Student Health Clinic
- McKerracher Centre Day Program
- Rural Clinics – Biggar, Humboldt, Kindersley, Lanigan, LaRonge, Outlook, Rosetown, Rosthern,
- West Side Community Clinic
- Northern Medical Services
We are a group of child and adolescent psychiatrists working within the Saskatoon Health Region. We provide psychiatric assessment to children, adolescents and their families. We are involved in teaching to medical students, trainees in psychiatry, paediatrics, and family medicine, and other health care professionals. We are also actively engaged in research of mental health involving children and adolescents.
Clinical Services:
- Psychiatric Assessment, Evaluation and Treatment to Children, Adolescents and their families
- An inpatient service with a 10-bed in-patient unit
- 24-hour Psychiatric Emergency Consultation and Assessment Service
- Consultation Liaison to Pediatrics
- Forensic Assessments
- Consultation services to residential treatment programs and group homes
- Work with Community Mental Health and Addictions Services
- Consultation services to Social Services on a case by case basis
We do not provide Psychological Assessment, Educational Assessments, & Custody and Access Assessments.
Forms:
WHO DAS 2 Children and Youth Form
Information for Parents
- The Referral: We understand that your child or adolescent has been referred for psychiatric assessment.
- Contact with Referral Source: When you go to your family physician for referral you will be asked to complete a family form called the family database and in addition a specific rating scale called the Who-Das. These are necessary for our assessment. It helps us to be better prepared for the assessment.
- School Information: In some cases, it is important to have information from the school. These forms will be given to you by your family physician, or sent from our office if they are required. Included with these forms will be a consent form to allow the school send information to us. This information is very helpful and important in helping us better assess your child.
- The Assessment: We understand that you may have worries, concerns and some apprehension about the assessment. The assessment will be completed by a trained child and adolescent psychiatrist with a team of residents working with us as well as senior medical students. Residents are specific postgraduate medical physicians training in family medicine, pediatrics, psychiatry and child psychiatry. On occasions there will be other individuals in the assessment. These individuals may be from other disciplines such as social work, psychology, healthcare and other disciplines and backgrounds. Everyone will follow all the standard confidentiality protocols.
- Confidentiality is very important for everyone concerned. Most importantly it is very necessary to reinforce that any information obtained will be protected in the most confidential manner to safeguard your child. Everyone working on the team follows the standard confidential privacy information act by the Saskatchewan Government called the HIPA (Health Information Privacy Act).
Access to information regarding the assessment:
- Consent Forms: When you come for the assessment you will be asked to complete a release of information form. This will determine who we would have permission to exchange information with such as your family physician and/or any other individuals such as schools. Most of the time it would be to have permission to collect information. Occasionally it may be to make specific recommendations about treatment. No information will be sent without your permission.
- Privacy and Confidentiality: we also ask you to respect the privacy and confidentiality of individuals that you might meet in the waiting room. Just as they are expected to respect your confidentiality and privacy the same is expected of you.
Dr. Anna Felstrom
Child & Adolescent Psychiatry Division Head
The Division of Forensic Psychiatry was established in February 2009 to organize the activities of substantial number of psychiatrists in the province who are involved in Forensic clincial practice, teaching of psychiatry residents, FMRs and medical students, and researching various aspects of Forensics.
The Division of Forensic Psychiatry offers a one-year PGY6 Forensic Psychiatry Training Program. The program is an accredited training program that follows the Royal College of Physicians and Surgeons of Canada training requirements in Forensic Psychiatry.
Clinical Services:
- Providing care to inpatients at the Regional Psychiatric Center in Saskatoon; the Forensic unit of the Saskatchewan Hospital North Battleford
- Providing care to patients at the Forensic outpatient clinic at Royal University Hospital and incarcerated patients at both Saskatoon Correctional Center and the Regina provisional correctional Center
- Court-ordered psychiatric assessments (Fitness to Stand Trial and Criminal Responsibility Assessments)
- Comprehensive care and services for people with serious mental illness who are placed under the jurisdiction of the Saskatchewan Review Board because they have been found not criminally responsible for their offense, or they have been deemed unfit to stand trial, on the account of having a serious mental illness
- Partnership with community services including probation, National Parole Board, Crisis Management, and Mental Health and Addictions
Dr. Stephen Adams, MD, FRCPC
Forensic Division Head
We are a group of three geriatric psychiatrists working at various locations throughout the city of Saskatoon. As part of the University of Saskatchewan College of Medicine and the Saskatoon Health Region, we provide psychiatric services to seniors with mental health problems, prioritizing those with multiple frailties including cognitive impairment. Especially for those with multiple medical comorbidities, we are increasingly working on a shared care model, in which the primary care physician retains the most responsible physician role, and we provide support and consultation. This model is not only necessary because of the shortage of dedicated geriatric psychiatrists, but is also best for the more frail patients, for whom psychiatric symptoms frequently reflect underlying medical disease.
We are involved in teaching to medical students, trainees in psychiatry, geriatric medicine, and family medicine, as well as other health care professionals, especially those providing care in nursing homes. We are also actively engaged in research of mental health involving older adults.
- Outpatient Geriatric psychiatry (RUH, SCH and private office)
- Inpatient Psychiatry (Dr. Prasad: Irene and Leslie Dubé Centre for Mental Health at RUH)
- Consultation-Liaison Psychiatry
- RUH (Dr. Prasad)
- SCH (Dr. Thorpe)
- SPH (Dr. L. Wanson)
- Long-term care ( Drs. Davidson, Prasad and Thorpe)
Featured Links:
Insight Podcast and CBC Blue Sky
With a goal of public outreach and education on mental health and wellness, we developed an in-house podcast in 2024 to discuss a wider range of issues for those who are interested in learning even more. Please visit our podcast at the link below.
INSIGHT INTO MENTAL HEALTH AND WELLNESS - DEPARTMENT OF PSYCHIATRY PODCAST
Since 2022, our Department members have been featured on CBC Radio's on the Blue Sky program. New episodes will be linked below.
pihtikwê podcast
pihtikwê means "welcome" in the Cree language. In this podcast, three leading First Nations psychologists, Dr. Brenda Restoule, Dr. Holly Graham and Dr. Alanaise Ferguson, welcome Indigenous psychologists and health leaders in the mental wellness fields to share their stories, knowledge, and lived experiences. Together they discuss how that relates to challenges and successes in navigating and working within systems of care, and strength-based and cultural approaches to healing.
Contact
Provincial Head's OfficeRoom 119 Ellis Hall, Royal University Hospital Michelle Haley Phone: (306) 844-1310 |
For clinical bookings, please use the phone number for your specific psychiatrist -- many of which can be found on Google or on our faculty listing.
|
Undergraduate Medical EducationRoom 110 Ellis Hall, Royal University Hospital Rozan Dudhwala Phone: (306) 844-1312 |
Postgraduate Medical EducationRoom 110 Ellis Hall, Royal University Hospital Nadine Loran Phone: (306) 844-1080
|
Communications OfficeRoom 119 Ellis Hall, Royal University Hospital Dallas Carpenter Email: psychiatry.communications@usask.ca
|
Research OfficeRoom 365 Ellis Hall, Royal University Hospital Dr. Mariam Alaverdashvili Email: research.psychiatry@usask.ca Phone: (306) 844-1302
|
|
Find us at our resident-managed Instagram account!
|
|