About Us
What is a Physiatrist?
Physicians trained in the specialty of Physical Medicine and Rehabilitation (PM&R) are called Physiatrists (fizz eye' uh trists).
Physiatry is the branch of medicine emphasizing the prevention, diagnosis, treatment, and rehabilitation of disorders, particularly those of the neuromusculoskeletal, cardiovascular, and pulmonary systems, that may produce temporary or permanent impairment.
Physiatry is unique among medical fields in that its area of expertise is the functioning of the whole patient, as compared with a focus on an organ system or systems.
Physiatrists treat conditions of the bones, muscles, joints, brain, and nervous system, which can affect other systems of the body and limit a person's ability to function.
The Physiatrist can help to improve a person's functional capabilities by medical treatment and organizing and integrating a program of rehabilitation therapy such as physical, occupational, speech therapies, psychological, social nursing, prosthetic, orthotic, engineering and vocational services.
--Definition from Association of Academic Physiatrists and Canadian Association of Physical Medicine & Rehabilitation--
Mission Statement
The mission of the Department of Physical Medicine and Rehabilitation at the University of Saskatchewan is to provide excellent patient care, education, and research in the field of Physical Medicine and Rehabilitation, leading to improvement in function, independence, health, and quality of life for each individual served.
We provide holistic interdisciplinary assessment and rehabilitation services to patients and families, and we are committed to advancing knowledge of the art and science of medical rehabilitation.
Programs
The Department of Physical Medicine and Rehabilitation (PM&R) at the University of Saskatchewan offers clinical clerkship electives at both the Saskatoon City Hospital in Saskatoon, Saskatchewan, and the Wascana Rehabilitation Centre in Regina, Saskatchewan. Our academic residency program operates out of both sites, allowing clerks a broad exposure to the daily responsibilities of academic physiatrists and residents.
Clerks who are interested in a career in PM&R or a complimentary specialty such as Neurology, Orthopedics, Rheumatology, Neurosurgery or Family Medicine are encouraged to apply. Students will have the opportunity to their history taking and physical exam skills in core PM&R domains such as musculoskeletal, neurological, acquired brain injury, stroke rehabilitation, spinal cord injury, multiple sclerosis, and prosthetics and orthotics and others. Acute care consults and rehabilitation inpatient ward exposure will provide a “day in the life of Physiatry” involving history, examination, diagnosis and treatment. Neuromuscular assessment and diagnosis is provided in the department allowing the student exposure to nerve conduction studies (NCS) and needle electromyography (EMG)
And elective schedule will be created based on the clerks’ personal interests and basic physiatry learning objectives. A minimum of 1 week is required but up to 4 weeks is permitted. Both Regina and Saskatoon sites will provide a flexible elective. A combination of outpatient clinical, inpatient ward, consultation service, and formal teaching at the resident academic half day will make up the bulk of the rotation.
Please contact pmr@usask.ca for more information.
The University of Saskatchewan Department of Physical Medicine & Rehabilitation is a provincial program that provides a flexible opportunity to take advantage of the best training opportunities in Saskatoon and Regina as well as some opportunities to experience one or more regional centers.
We have integrated support for research with access to research scientists in both cities. We have strong working relationships with neurosciences, rheumatology and orthopedics. Both centres have established services in the core rehabilitation areas of stroke, spinal cord injury, brain injury and amputation.
In Regina at Wascana Rehabilitation Centre, we have all core rehabilitation services on one site including inpatient and outpatient services, prosthetics and orthotics, specialized seating and services for children with such diagnoses as cerebral palsy and spina bifida. At Saskatoon City Hospital there are inpatient and outpatient rehabilitation services, in addition to two community physiatrists with a mix of musculoskeletal and electrodiagnostic medicine. There is the opportunity to work with off site pediatric subspecialists as well as teams managing cerebral palsy, spina bifida and other neuromuscular diseases in addition to orthotics and prosthetics. As there is currently no certified pediatric physiatrist in Saskatchewan, we have an affiliation agreement in place with the University of Calgary where we require and support one block of pediatric rehabilitation.
Our two tertiary rehabilitation centres in Saskatoon and Regina serve a provincial population of just over one million. We feel the single program distributed between both cities offers the best of flexibility, personalized attention and practical experience. There is excellent support from the College of Medicine to support this distributed model. We have a strong focus on neurological and musculoskeletal anatomy reinforced by five half days per year in the College of Medicine anatomy lab guided by an anatomist and physiatrist. We are building our expertise for integrating ultrasound into chemodenervation and musculoskeletal procedures. We have also initiated optional EMG and ultrasound teaching rounds in addition to our regular academic teaching program.
Please contact pmr@usask.ca for more information.

Left to Right: Dr. Katherine Knox, Julie Gillis, Dr. Shane Wunder, Dr. Brendan Kushneriuk
Photo taken at the PGME Awards Ceremony, honoring the Program Director of the Year, Dr. Shane Wunder.
Research
Overview
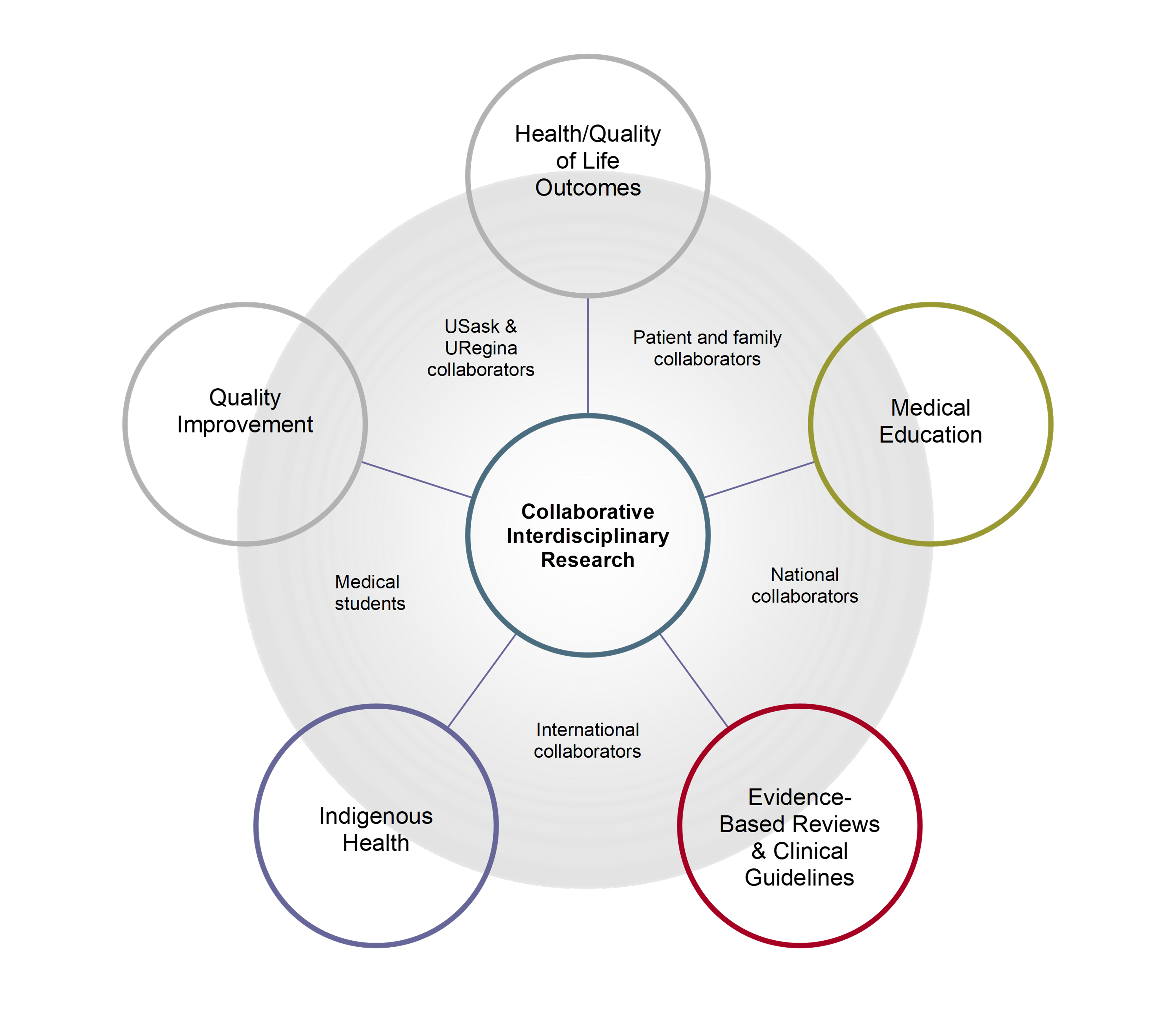
Physical Medicine and Rehabilitation is a collaborative field of practice. Accordingly, we conduct collaborative interdisciplinary research in health/quality-of-life outcomes, medical education, evidence-based reviews and clinical guidelines, Indigenous health, and healthcare quality improvement with patient and family partners, medical students, and local, national, and international researchers.
Each of our residents complete at least one scholarly project during their residency. This contributes to a culture of research in our department and advances scholarly activity. We aim to equip our residents to be keen and aware users of research literature and competent and responsible research partners.
Research Model for Department of Physical Medicine and Rehabilitation, University of Saskatchewan
This page contains some recent publications that members of our department have published.
Papers 2025-2026
- Donkers S, Bayley M, Bruno TR, Marrie RA, Simpson R, Smyth P, Knox K. Building bridges: establishing a multiple sclerosis rehabilitation research and clinical knowledge mobilization strategy. NeuroRehabilitation. Available online 29 Aug 2025. https://doi.org/10.1177/10538135251365102
- Gaid D, Neufeld J, Boden C, Knox KB, Bayley M, Bruno TR, Simpson R, Donkers SJ. Rehabilitation interventions for improving gait for people with multiple sclerosis: A scoping review of reviews. Mult Scler Related Disord. 2025; 104:106784. https://doi.org/10.1016/j.msard.2025.106784
- Hong HA, Parsons J, Xu J, Walden K, Fallah N, Cheng CL, Attabib N, Christie SD, Craven BC, Fehlings MG, Fourney DR, Ho C, Julien L, Kwon BK, Linassi AG, Loyola-Sanchez A, Moganathas S, Paquet J, Sreenivasan V, Mac-Thiong JM, Townson A, Tsai EC, Urquhart J, Whelan A, Noonan VK, the ISNCSCI Working Group. An Evaluation of International Standards for Neurological Classification of Spinal Cord Injury (ISNCSCI) performance within the Canadian SCI Network. Top Spinal Cord Inj Rehabil. 2025; 31(3): 15–36. https://doi.org/10.46292/sci25-00011
- Scandiffio J, Langer LK, Senthilnathan V, Feng G, Sureshkumar A, Bromberg M, Babineau J, Donkers SJ, Knox KB, Bruno T, Walker LAS, Bayley MT, Simpson R. Effects of psychological therapies in people with multiple sclerosis: a systematic review and network meta-analysis of randomized controlled trials. J Neurol. 2025; 272: 584. https://doi.org/10.1007/s00415-025-13315-6
- Schellenberg KL, Caspar-Bell G, Ellis C, Johnston W, King A, King M, Korngut L, Kushneriuk B, Lavoie AJ, McGonigle R, Newton J, O’Connell C, Shoesmith C, Suchowersky O, Warman-Chardon J, Wunder S, Pfeffer G. Best practice recommendations for the clinical care of spinal bulbar muscular atrophy. Can Med Assoc J. 2025, 22;197: E987-E999. https://doi.org/10.1503/cmaj.250180
- Walker LAS, Finlayson M, Cameron J, Donkers SJ, Knox K, Mayo N, Ploughman M, Canlas K, Jacksch M, Liu S, Pilutti L. A conceptual approach to comprehensive interdisciplinary cognitive rehabilitation: A description using the TIDieR-Rehab Framework. Mult Scler Relat Disord. 2025. https://doi.org/10.1016/j.msard.2025.106783
Papers 2024-2025
- Dionne A, Mac-Thiong JM, Hong HA, Kurban D, Xu J, Humphreys S, Bailey C, Barthelemy D, Christie S, Fourney D, Linassi AG, Loyola-Sanchez A, Paquet J, Sreenivasan V, Townson A, Tsai E, Noonan VK, Richard-Denis A, the RHSCIR Network. Is the level of consent to a national research registry associated with patient outcomes following traumatic spinal cord injury? A population-based study from the Rick Hansen Spinal Cord Injury Registry (RHSCIR). Am J Phys Med Rehabil. 2025; 104(2): 130-137. https://doi.org/10.1097/PHM.0000000000002549
- Donkers SJ, Evans C, Levin MC, Ives K, Le H, Lim HJ, Knox KB. Individualized physiotherapy and activity coaching in multiple sclerosis (IPAC-MS): Results of a randomized controlled trial. Arch Phys Med Rehabil. 2025; 106: 1145-1154. Available online 15 Feb 2025. https://doi.org/10.1016/j.apmr.2025.02.005
- Knox KB, Islam A, Le T, Donkers SJ, Evans C, Lim HJ. Physical activity in multiple sclerosis: Real-world data From Saskatchewan, Canada. Int J MS Care. 2025; 27: 42–49. https://doi.org/10.7224/1537-2073.2024-006
- Peltonen J, Benson S, Kraushaar J, Wunder S, Mang C. Stroke survivors with limited walking ability have unique barriers and facilitators to physical activity. Disabil Rehabil. 2025; 47: 4664–4672. Available online 17 Jan 2025. https://doi.org/10.1080/09638288.2025.2453639
- Shukla K, Lanovaz JL, Farthing JP, Linassi G, Oates AR. Reliability and Error in Step Parameters and Balance Measures Across Different Walking Styles in Adults. Preprint available at SSRN: http://dx.doi.org/10.2139/ssrn.5130977
Papers 2023-2024
- Calver R, Cudlip A, Dickerson CR, Mondal P, Butcher S, Kim SY. A comparison of isometric and isokinetic normalization methods for electromyographic data from sub-regions of supraspinatus and infraspinatus during dynamic tasks. Int Biomech. 2023; 10(1): 1-9. https://doi.org/10.1080/23335432.2023.2210634
- Chin PYK, Regan W, Plausinis D, Zarzour Z, Leung F, Johnston K, Lim B, Sasyniuk T. A multicenter, randomized controlled trial comparing a second-generation uncemented trabecular metal-backed vs. cemented polyethylene glenoid component in total shoulder arthroplasty: 5-year results. J Shoulder Elbow Surg. 2024; 33(5): 1004-1016. https://doi.org/10.1016/j.jse.2023.12.004
- Feng G, Posa S, Sureshkumar A, Simpson S, Bruno T, Morrow SA, Donkers S, Knox K, Feinstein A, Bayley M, Munce S, Simpson R. Experiences of people with multiple sclerosis and clinicians in using cognitive behavioural therapies for hidden symptoms: a systematic review and meta-aggregation. J Neurol. 2024; 271: 1081-1107. https://doi.org/10.1007/s00415-023-12116-z
- Patrick S, Knox KB, Evans C, Levin M, Linassi G, Poliakov I, Rajput A, Donkers SJ. ‘NeuroSask: Active and Connect’ - A virtual chronic disease management program for individuals with a neurological condition. Front Neurol. 2024; 15. https://doi.org/10.3389/fneur.2024.1332859
Papers 2022-2023
- Kassam F, Lim B, Afroz S, Boissonnault È, Reebye R, Finlayson H, Winston P. Canadian physicians’ use of intramuscular botulinum toxin injections for shoulder spasticity: a national cross-sectional survey. Toxins. 2023; 15(1): 58. https://doi.org/3390/toxins15010058
- Kelly R, Leung G, Lindstrom H, Wunder S, Jaime CY. Virtual objective structured clinical examination experiences and performance in physical medicine and rehabilitation residency. Am J Phys Med Rehabil. 2022 Oct 1; 101(10): 947-53. https://doi.org/10.1097/PHM.0000000000001942
- Knox KB, Nickel D, Donkers SJ, Paul L. Physiotherapist and participant perspectives from a randomized-controlled trial of physiotherapist-supported online vs. paper-based exercise programs for people with moderate to severe multiple sclerosis. Disabil Rehabil. 2022; 45(7): 1147-1153. https://doi.org/10.1080/09638288.2022.2055159
Online resources 2021-2022
- Abdulhadi E, Ireland D, Simpson R, Morrow SA, Le E, Donkers S, Knox KB, on behalf of the MSBEST Team. Cognitive impairment: non-pharmacological rehabilitation interventions. Multiple Sclerosis Best Evidence-Based Strategies and Treatment/Therapies for Rehabilitation. Version 1.0. 2022. p 1-219. https://kite-uhn.com/msbest/modules/cognitive-non-pharmacological
- Morrow S, Mirkowski M, Duff W, Knox K, on behalf of the MSBEST Team. Cognitive impairment: pharmacological interventions. Multiple Sclerosis Best Evidence-Based Strategies and Treatment/Therapies for Rehabilitation. Version 1.0. 2021. p 1-107. https://kite-uhn.com/msbest/modules/cognitive-pharmacological
Papers 2021-2022
- Alavinia SM, Jetha A, Hitzig SL, McCauley D, Routhier F, Noonan VK, Linassi G, Farahani F, Omidvar M, Jeyathevan G, Craven BC. Development of employment indicators to advance the quality of spinal cord injury rehabilitation care: SCI-High Project. J Spinal Cord Med. 2021; 44(sup1): S118-133. https://doi.org/10.1080/10790268.2021.1955205
- Andrushko JW, Gould L, Renshaw DW, Forrester S, Kelly ME, Linassi G, Mickleborough M, Oates A, Hunter G, Borowsky R, Farthing JP. Ipsilesional motor cortex activation with high force unimanual handgrip contractions with the less-affected limb in participants with stroke. Neuroscience. 2022; 483: 82-94. https://doi.org/10.1016/j.neuroscience.2021.12.011
- Essien SK, Kopriva D, Linassi AG, Zucker-Levin A. Trends of limb amputation considering type, level, sex and age in Saskatchewan, Canada 2006-2019: an in-depth assessment. Arch Public Health. 2022; 80: 10. https://doi.org/10.1186/s13690-021-00759-1
- Essien S, Linassi AG, Farnan C, Collins K, Zucker-Levin A. The influence of primary and subsequent limb amputation on the overall rate of limb amputation in Saskatchewan, Canada, 2006-2019: a population-based study. BMC Surg. 2021; 21: 385. https://doi.org/10.1186/s12893-021-01381-2
- Essien SK, Linassi AG, Larocque M, Zucker-Levin A. Incidence and trends of limb amputation in First Nations and general population in Saskatchewan, 2006-2019. PLOS ONE. 2021; 16(7): e0254543. https://doi.org/10.1371/journal.pone.0254543
- Hitzig SL, Jeyathevan G, Farahani F, Noonan VK, Linassi G, Routhier F, Jetha A, McCauley D, Alavinia SM, Omidvar M, Craven BC. Development of community participation indicators to advance the quality of spinal cord injury rehabilitation: SCI-High Project. J Spinal Cord Med. 2021; 44(sup1): S79-93. https://doi.org/10.1080/10790268.2021.1955204
- Jeyathevan G, Jaglal SB, Hitzig SL, Linassi G, Mills S, Noonan VK, Anzai K, Clarke T, Wolfe D, Bayley M, Aslam L, Farahani F. Alavinia SM, Omidvar M, Craven BC. Conception and development of self-management indicators to advance the quality of spinal cord injury rehabilitation: SCI-High Project. J Spinal Cord Med. 2021; 44(sup1): S94-S117. https://doi.org/10.1080/10790268.2021.1961054
- Saini A, Cochran C, Zucker-Levin A, Donkers SJ, Kumar P, Knox KB, MacPherson J, Salapa H, Levin MC. A tripartite knowledge translation program: innovative patient-centered approach to clinical research participation for individuals with multiple sclerosis. Mult Scler Int. 2021. Article ID: 5531693. https://doi.org/10.1155/2021/5531693
- Sarpong-Kumankomah S, Knox KB, Kelly ME, Hunter G, Popescu B, Nichol H, Kopciuk K, Ntanda H, Gailer J. Quantification of human plasma metalloproteins in multiple sclerosis, ischemic stroke and healthy controls reveals an association of haptoglobin-hemoglobin complexes with age. PLoS ONE. 2021; 17(1): e0262160. https://doi.org/10.1371/journal.pone.0262160
- Stacey A, D’Eon M, Andersen M, Koehncke N, Campoli J, Thompson G, Riou K. Warning: medical education is hazardous to your mental health. Medical students should make an informed decision to begin and continue training. Can Med Ed J. 2022 Jun. 14; 13(5): 39-44. https://doi.org/10.36834/cmej.73959
- Tauh S, Nickel D, Thorpe L, Brown J, Linassi G. Perspectives on medical assistance in dying amongst persons with traumatic spinal cord injury: A qualitative study. Spinal Cord. 2022; 60: 465-469. https://doi.org/10.1038/s41393-022-00793-y
Papers 2020-2021
- Bone MD, Arora T, Musselman KE, Lanovaz JL, Linassi GA, Oates AR. Investigating proactive balance control in individuals with incomplete spinal cord injury while walking on a known slippery surface. Neurosci Lett. 2021 Apr 1; 749: 135744. https://doi.org/10.1016/j.neulet.2021.135744
- Collins K, Linassi G, Zucker-Levin A. A focus group- and patient-driven study to understand patient and healthcare provider perspectives of services for amputees. Physiotherapy Canada. 2021; 73(3): 244-251. https://doi.org/10.3138/ptc-2019-0054
- D'Eon M, Thompson G, Stacey A, Campoli J, Riou K, Andersen M, Koehncke N. The alarming situation of medical student mental health. Can Med Educ J. 2021 Jun 30; 12(3): 176-178. https://doi.org/10.36834/cmej.70693
- Hodgkinson V, Lounsberry J, M’Dahoma S, Russell A, Benstead T, Brais B, Campbell C, Johnston W, Lochmuller H, McCormick A, Nguyen CT, O’Ferrall E, Oskoui M, Briemberg H, Bourque P, Botez S, Cashman N, Chapman K, Chrestian N, Crone M, Dobrowski P, Dojeiji S, Dowling JJ, Dupre N, Genge A, Gonorazky H, Grant I, Hasal S, Izenberg A, Kalra S, Katzberg H, Krieger C, Leung E, Linassi G, Mackenzie A, Mah JK, Marrero A, Massie R, Matte G, McAdam L, McMillan H, Melanson M, Mezei MM, O’Connell C, Pfeffer G, Phan C, Plamondon S, Poulin C, Rodrigue X, Schellenberg K, Selby K, Sheriko J, Shoesmith C, Smith G, Taillon M, Taylor S, Venance S, Warman-Chardon J, Worley S, Zinman L, Korngut L. The Canadian Neuromuscular Disease Registry 2010-2019: A decade of facilitating clinical research through a nationwide pan-neuromuscular disease registry. J Neuromuscul Dis. 2021; 8(1): 53-61. https://doi.org/10.3233/jnd-200538
- Inglis T, Banaszek D, Rivers CS, Kurban D, Evaniew N, Fallah N, Waheed Z, Christie S, Fox R, Mac-Thiong J-M, Ethans K, Ho C, Linassi AG, Ahn H, Attabib N, Bailey C, Fehlings MG, Fourney DR, Paquet J, Townson A, Tsai E, Cheng CL, Noonan VK, Dvorak MF, Kwon BK. In-Hospital Mortality for the Elderly Suffering Acute Traumatic Spinal Cord Injury. J Neurotrauma. 2020; 37(21): 2332-2342. https://doi.org/10.1089/neu.2019.6912
- Saini A, Bach K, Poliakov I, Knox KB, Levin MC. Magnetic Resonance Imaging of spinal cord lesions in a cohort of patients with multiple sclerosis in Saskatchewan, Canada. Int J MS Care. 2021; 23(2): 47-52. https://doi.org/10.7224/1537-2073.2019-081
- Sessford JD, Locke SR, Cary MA, Flora PK, Knox K, Brawley LR. Effect of group counseling plus tailored exercise on mobility function in multiple sclerosis. Int J MS Care. 2021; 23(2): 66-72. https://doi.org/10.7224/1537-2073.2019-066
- Siemens M, Wunder S, Kraushaar J, Mortimer JA, Siddiqui M, Kane K. Hip surgery and radiology reporting for children with cerebral palsy prior to initiation of a hip surveillance program. J Pediatr Rehabil Med. 2021; 14(2): 257-263. https://doi.org/10.3233/prm-201506
Resources
Program Administration and Collaboration
- UofS Rehab SharePoint:
- Academic Half Day Schedule and link to Zoom meetings contained within.
- Please contact pmr@usask.ca if you do not have access and require a copy.
Evaluation Forms
Other Resources
Contact
Saskatoon Rehabilitation Centre
Saskatoon City Hospital
701 Queen St
Saskatoon SK
S7K 0M7
Reception Tel: 306-655-8175
Fax: 306-655-8813
Wascana Rehabilitation Centre
2180 - 23rd Avenue
Regina SK
S4S 0A5
Appointment Coordinator Tel: 306-766-5521
Outpatient Clinic Nurse Tel: 306-766-5514
Admin Assistant Tel: 306-766-5402
Fax: 306-766-7442
